Skin, Hair & Beauty
Wet Shoes, Itchy Toes, and the Wrong Cream
Rainy weeks can leave feet damp, itchy and peeling. The right treatment is usually simple, but the wrong cream can drag the problem out.
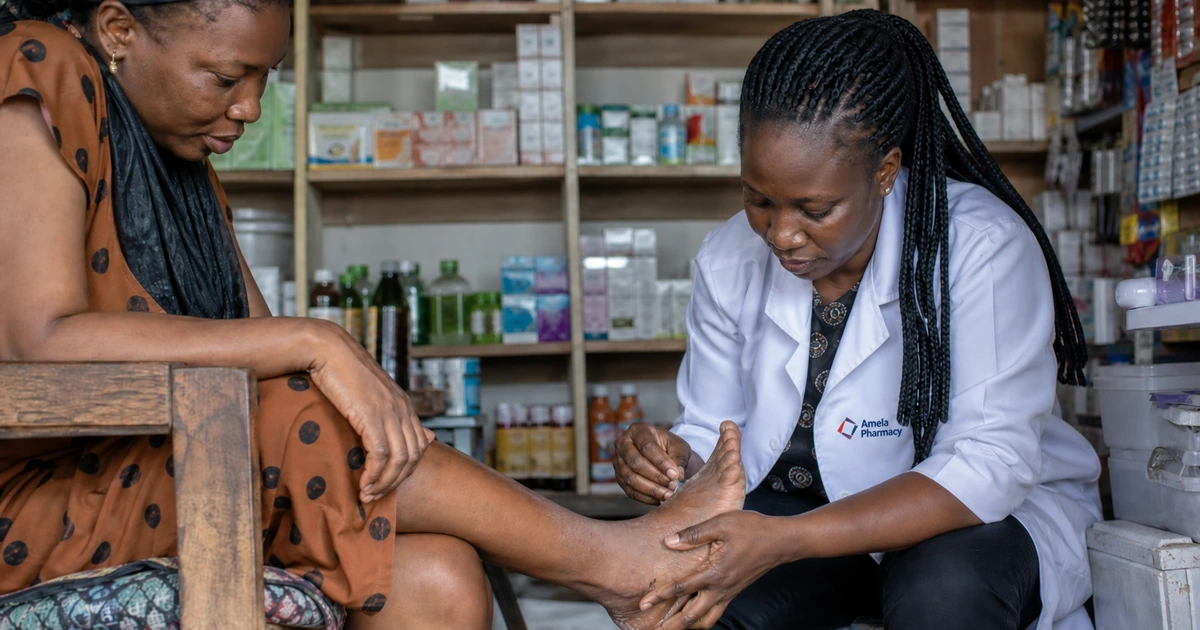
Reviewed by: Amela Pharmacy team, Uyo Last updated: 6 Apr 2026
Rainy mornings have a way of following you into the rest of the day. One keke ride, one wet pair of socks, one long stretch in closed shoes, and by evening the skin between your toes is itching badly.
We see this often at the counter once the weather gets damp. Someone comes in asking for "any cream for itching." They already tried one random tube at home, the itching eased briefly, then the skin turned whiter, peelier, and more irritated.
That pattern can point to athlete's foot, a fungal skin infection. It is common, frustrating, and usually manageable. What keeps it hanging around is often not the fungus itself. It is starting with the wrong cream, stopping treatment too early, or putting damp feet back into the same shoes every day.
What athlete's foot usually looks like
Athlete's foot often starts between the toes. The skin may itch, burn, peel, crack, or look soft and whitish, especially after sweating or bathing. Some people notice dry scaling on the sole. Others get small blisters or soreness where the skin has split.
It does not always look dramatic. Sometimes it is just that stubborn itch that shows up again every evening after work. If you have been doing market runs in closed shoes, or your work or school shoes stayed damp after rain, that warm, wet space gives fungus exactly what it likes.
Not every foot rash is athlete's foot, though. Eczema, shoe irritation, bacterial infection, and some inflammatory rashes can look similar. That is why using whatever "anti-itch" cream is nearby can make things worse.
The cream mistake that makes it linger
A very common mistake is starting with a steroid cream, or one of those mixed rash creams that contains a steroid, before confirming what the rash is. A steroid can reduce redness and itching for a short time, so it may look like it is helping. Meanwhile, the fungus may keep spreading underneath. By the next week, the rash is wider, the skin is more irritated, and treatment is more stressful than it needed to be.
For straightforward athlete's foot, pharmacy antifungal treatment is often the right place to start. Creams, sprays, or powders may be used depending on the product and the area affected. Common antifungal ingredients include clotrimazole, miconazole, and terbinafine. The exact option matters less than using the right one properly and for long enough.
That last part matters a lot. People often stop treatment once the itching settles. That is how it comes back. If the instructions say use it for the full course, finish the course. Fungal skin infections are well known for looking better before they are truly gone.
A simple rainy-season foot routine
If the rash seems mild and localised, this home routine usually gives you the best chance of clearing it:
- Wash your feet and dry them well, especially between the toes. Patting is better than hard rubbing if the skin is cracked.
- Change out of damp socks quickly. If your feet sweat a lot, you may need a fresh pair during the day.
- Rotate your shoes so one pair has time to dry properly before you wear it again.
- Use the antifungal exactly as directed on clean, dry skin, and finish the course even when the area looks better.
- Keep a separate towel for your feet if possible, and wash socks regularly.
- Do not share slippers, socks, nail clippers, or towels.
- Try not to scratch. Fungal rashes can spread to other parts of the body.
If your shoes stay damp all the time, treatment becomes harder than it should be. During rainy weeks, it helps to get home, remove the insoles if you can, and leave the shoes to air properly before the next day. It sounds minor, but it makes a real difference.
What usually helps, and what usually does not
Helpful: keeping the area dry, using an antifungal as directed, and choosing shoes that do not trap heat all day.
Less helpful: thick ointments that hold moisture in, random cream combinations from the back of a drawer, and using treatment only on the days the itching annoys you.
If the skin is badly macerated, very soggy, or cracked between the toes, a pharmacist can help you choose a form that is easier to use. Powders or sprays may help with sweaty shoes, but they do not replace proper treatment when there is already an active fungal infection.
When to seek urgent help
Get urgent medical help if you notice any of these:
- rapid swelling, spreading redness, warmth, or severe pain in the foot or leg
- pus, foul-smelling discharge, or fever
- you cannot bear weight properly, or the skin is breaking down fast
- you have diabetes, poor circulation, or nerve problems and now have cracks, sores, or a new foot rash
- the rash is spreading widely, involves the nails or scalp, or you feel generally unwell
And if you have used a pharmacy antifungal properly for a couple of weeks with little or no improvement, stop guessing and get it checked. A foot rash that is not responding may not be athlete's foot at all, or it may need prescription treatment.
How to stop it coming back
Recurrence is the frustrating part. The rash clears, life gets busy, and before long the same damp-shoe routine is back.
A few habits can lower the chances:
- Wear clean socks daily and change them sooner if they get wet.
- Let shoes dry fully before wearing them again.
- Choose footwear that allows some air movement when you can.
- Keep feet clean and dry after bathing.
- Avoid walking barefoot in shared bathrooms, hostels, or changing areas.
- Check children's feet too if they spend long days in enclosed school shoes.
A quick word on home remedies: if it stings, burns, or leaves the skin more irritated, stop. "Strong" is not the same as effective. After a long day of NEPA drama, wet floors, and general stress, your feet are not the place to start experimenting.
A sensible next step
If you think it may be athlete's foot, keep it simple: treat early, keep the feet dry, and do not start with a steroid cream unless a clinician has confirmed the rash. Most mild cases improve with the right pharmacy treatment and better foot habits. The longer it sits in damp shoes, the more stubborn and annoying it gets.
Disclaimer
This article is for general education and does not replace a proper assessment by a pharmacist or clinician. If you are unsure what the rash is, if symptoms are severe, or if you have diabetes or a weakened immune system, seek professional care early.
A small foot itch is much easier to sort out before it turns into a bigger problem.
No comments yet. Login to start a new discussion Start a new discussion